Knockout iPSC Cell line

Introduction
Many serious diseases cannot be cured by medicines, such as heart failure, Late Stage Diabetes, hemophilia, myeloma, End-Stage Cirrhosis, etc. The best method is allogeneic transplantation. However, due to the limited donors and the risk of immune rejection, researchers are dedicated to finding more efficient and safer treatment besides allogeneic transplantation. Induced pluripotent stem cells (iPSCs) can be derived from the body cells of the patients themselves, which eliminates the risk of immune rejection, and has the potential of differentiation into different cells. Transplantation of cells derived from iPSC, such as cardiomyocytes, hepatocytes, neurocytes, T cells, hematopoietic stem cells (HSCs) and pancreatic cells, is possible to solve many medical problems.
The differentiation of liver cells induced by iPSC can alleviate the shortage of sources in liver transplantation and hepatocyte transplantation, which is more conducive to basic and clinical research. In addition, the induced hepatocyte could be used as a tool to simulate and study liver diseases and screen the hepatotoxicity of drugs in the future.
Neural stem cells differentiated from iPSC can be used to
generate cell models of nervous system diseases. This
approach avoids ethical problems and immune rejection, and
is an ideal way to obtain NSC in vitro.
iPSC can differentiate into neuron under appropriate
conditions. For example, differentiation into motor neurons
(MN) provides the possibility for the treatment and research
of MN injury diseases such as Amyotrophic lateral sclerosis
(ALS) and Spinal muscular atrophy (SMA).
iPSC can differentiate into T cell. The CAR-T cell therapy developed on the basis of iPSC has a safer and more effective pharmacological activity. iPSCs based CAR-T cells can be used in T cell immunotherapy without the limitation of Allograft rejection.
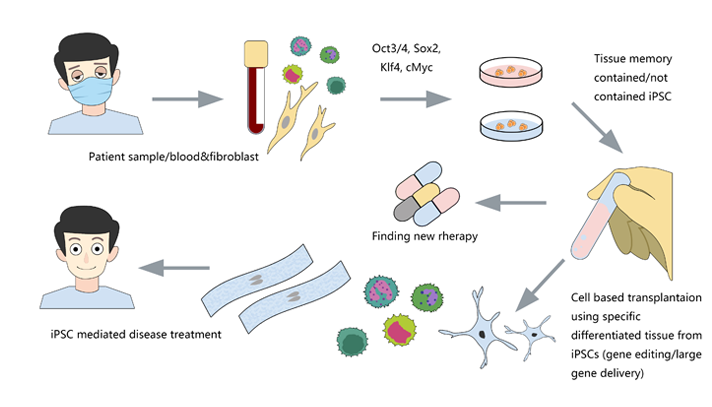
Ubigene’s iPSC platform:
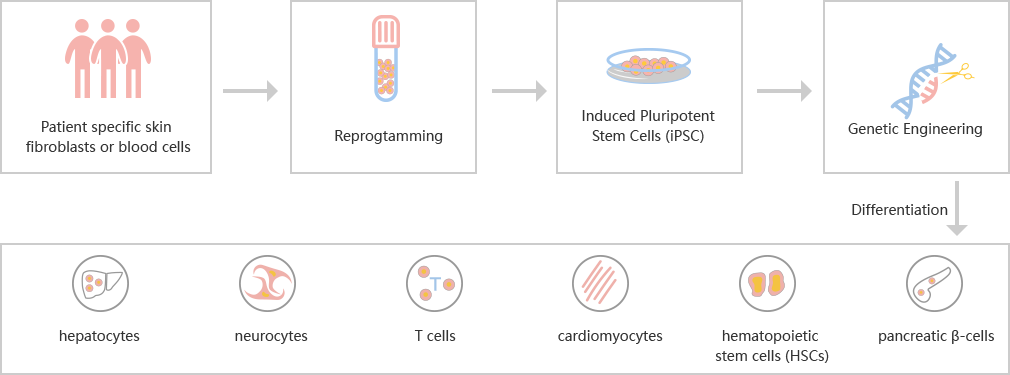
Reprogramming services
By transferring transcription factors, such as Oct3/4、Sox2、c-Myc and KlF4, somatic cells could be reprogrammed into iPSC with the potential of proliferation and differentiation.
Steps of iPSC reprogramming:
- Vectors carrying transcription factors will be transferred into somatic cells to reprogram into iPSC;
- iPSC validation: genotyping and phenotyping.
Gene editing service
The success rate of gene editing in human iPSC is lower because, unlike tumor cell lines, iPSC does not have the characteristics of chromosomal abnormality and strong ability of DNA repair. CRISPR/Cas9 has the advantages of high efficiency, easy to construct and low toxicity in human cells, so it is the most common method in iPSC genome editing. EZ-editor™ optimizes the targeting efficiency, greatly improve the efficiency of DSB and homologous recombination in iPSCs.
1. Knockout
EZ-editor™ gene knockout iPSC cell line: gRNA and Cas9 are transferred into iPSCs by nucleofection. After drug screening, single clones would be generated. Positive clones would be validated by sequencing.
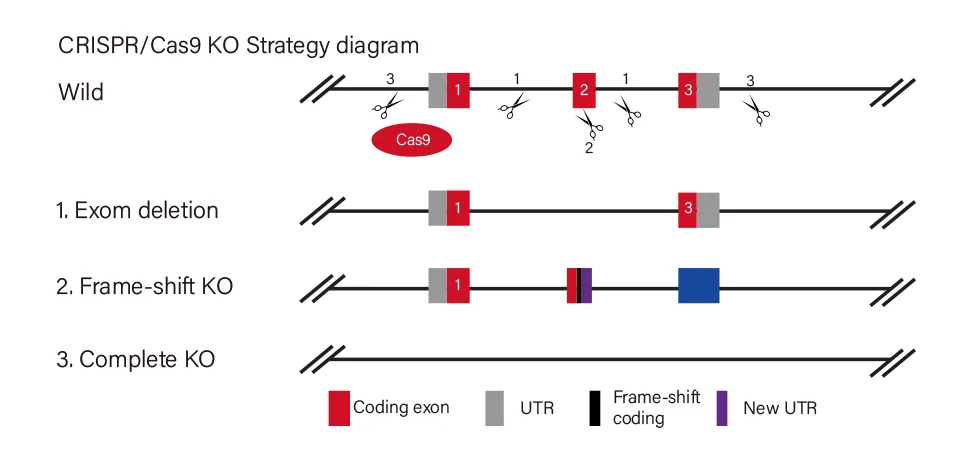
| Type | Strategy | Application |
| Short fragment removal | Guide RNAs target introns at both sides of exon 2 and the number of bases in exon 2 is not a multiple of 3, which can cause frame-shift mutation. | Study of gene function through gene defect |
| Frame-shift mutation | Guide RNA targets the exon, and the base number of deletion is not a multiple of 3. After knockout, frame-shift mutation would cause gene knockout. | |
| Large fragment removal | Complete removal of the coding sequence to achieve gene knockout. |
Case Study:
The limited T cells and the difficulty of proliferation is the main obstacle of T-cell immunotherapy, which can be overcome by using pluripotent stem cells with proliferation and differentiation ability to generate T-iPSC with antigen specificity. Strict antigen specificity is essential for safe and effective T-cell immunotherapy. However, in the process of double-positive CD4/CD8 differentiation, the rearrangement of the T-cell receptor (TCR) α chain will lose antigen specificity. This TCR rearrangement was prevented by removing the recombinant enzyme gene (RAG2) in T-iPSCs with CRISPR/Cas9. Xenotransplantation of CD8αβ-T cells with stable TCR can effectively inhibit tumor growth in disease models. This contributes to a safe and effective T-cell immunotherapy.
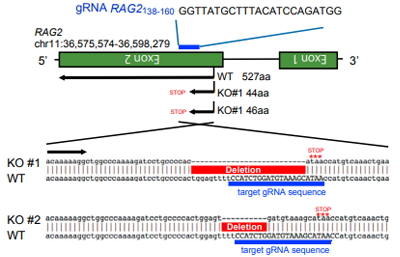
gRNA sequence and RAG2ockout sequence. The positive clones have frameshift mutations in the designated RAG2.

Comparison of the binding ability of WT and RAG2 knockout T-iPSCs to dextramer. RAG2-/- T-iPSCs differentiated into CD8αβ cells expressing stable TCR, while 40% of RAG2wt/wt-iPSC derived CD8αβ cells lost antigen specificity.
Reference:
Minagawa, Atsutaka, et al. "Enhancing T cell receptor stability in rejuvenated iPSC-derived T cells improves their use in cancer immunotherapy." Cell Stem Cell 23.6 (2018): 850-858.
2. Point Mutation
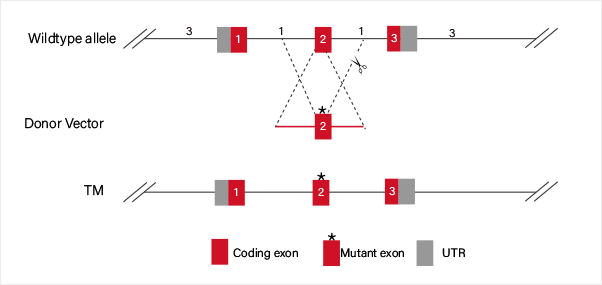
Case Study:
Disease model generation
ssODN carrying point mutation which replaces the WT sequence
by HDR.
Disease model rescuing
ssODN carrying WT sequence which replaces the mutated site
by HDR.

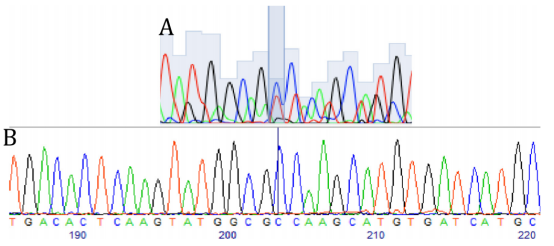
A) Heterozygous c.236C>T substitution in the mother line previously published.
B) Successful correction of the point mutation (T>C).
Reference:
Pires, C., Schmid, B., Petræus, C., Poon, A., Nimsanor, N., Nielsen, T. T., ... & Freude, K. K. (2016). Generation of a gene-corrected isogenic control cell line from an Alzheimer's disease patient iPSC line carrying a A79V mutation in PSEN1. Stem cell research, 17(2), 285-288.3. Gene Knock in
EZ-editor™ Gene Knockin iPSC: iPSC would be co-transfected with gRNA, Cas9 and donor vector by electroporation. After drug screening, single clones would be generated. Positive clones would be validated by sequencing.
Knockin Strategies:
Disease model generation
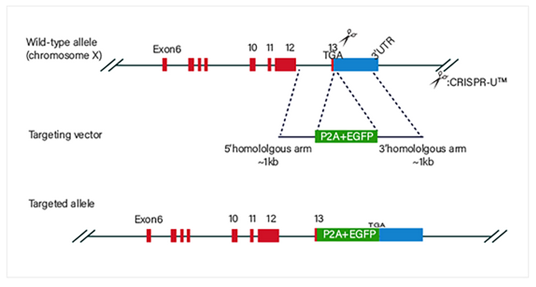
Safe harbor knockin:
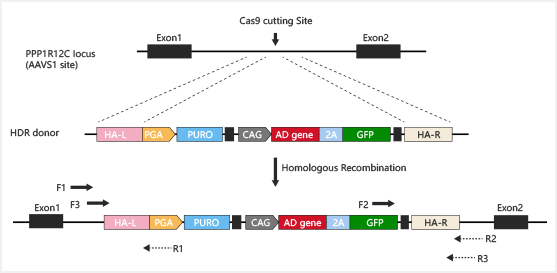
Case Study:
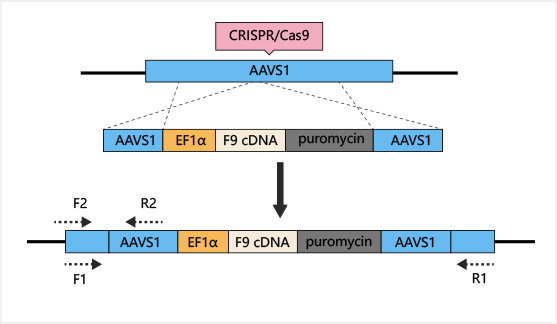
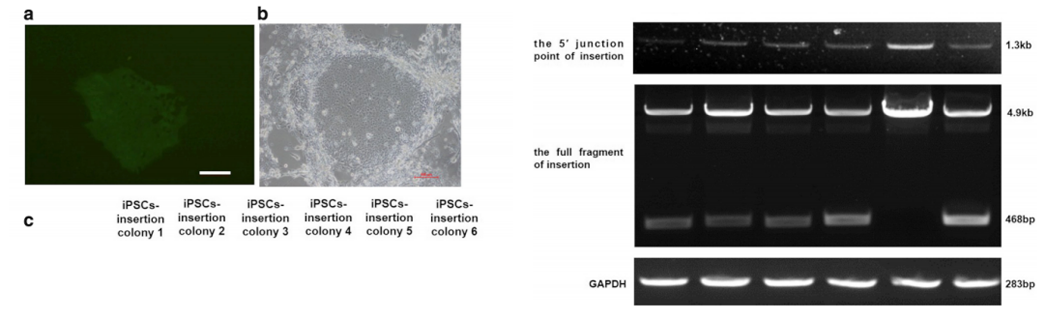
Reference:
Lyu, Cuicui, et al. "Targeted genome engineering in human induced pluripotent stem cells from patients with hemophilia B using the CRISPR-Cas9 system." Stem cell research & therapy 9.1 (2018): 92.iPSC differentiation
Differentiation Process




